close
keyboard_arrow_left
Solutions
close
keyboard_arrow_left
Products
close
-
Smart Beds & Surfaces keyboard_arrow_right
-
Patient Monitoring keyboard_arrow_right
-
Care Communications keyboard_arrow_right
-
Safe Patient Handling & Mobility keyboard_arrow_right
-
Healthcare Furniture keyboard_arrow_right
-
Non-Invasive Respiratory Therapy keyboard_arrow_right
-
Surgical Workflow & Precision Positioning keyboard_arrow_right
-
Procedural Connectivity keyboard_arrow_right
-
Diagnostic Cardiology keyboard_arrow_right
-
Physical Exam & Diagnostics keyboard_arrow_right
-
Vision Screening & Diagnostics keyboard_arrow_right
-
Veterinary & Animal Health keyboard_arrow_right
-
View All
Surgical Workflow & Precision Positioning
View All
- Equipment Booms, Pendants
- Surgical & Examination Lights
- Precision Positioning Table Accessories
- Surgical Tables
keyboard_arrow_left
Services
close
-
SmartCare™ Services keyboard_arrow_right
-
Care Communications Service keyboard_arrow_right
-
Financial Services keyboard_arrow_right
-
Therapy Rental keyboard_arrow_right
-
Replacement Parts keyboard_arrow_right
-
Construction Solutions keyboard_arrow_right
-
Customer Experience Centers keyboard_arrow_right
-
View All
keyboard_arrow_left
Knowledge
close
keyboard_arrow_left
Profile
close
- Advancing Connected Care
- Education and Evidence
- Article
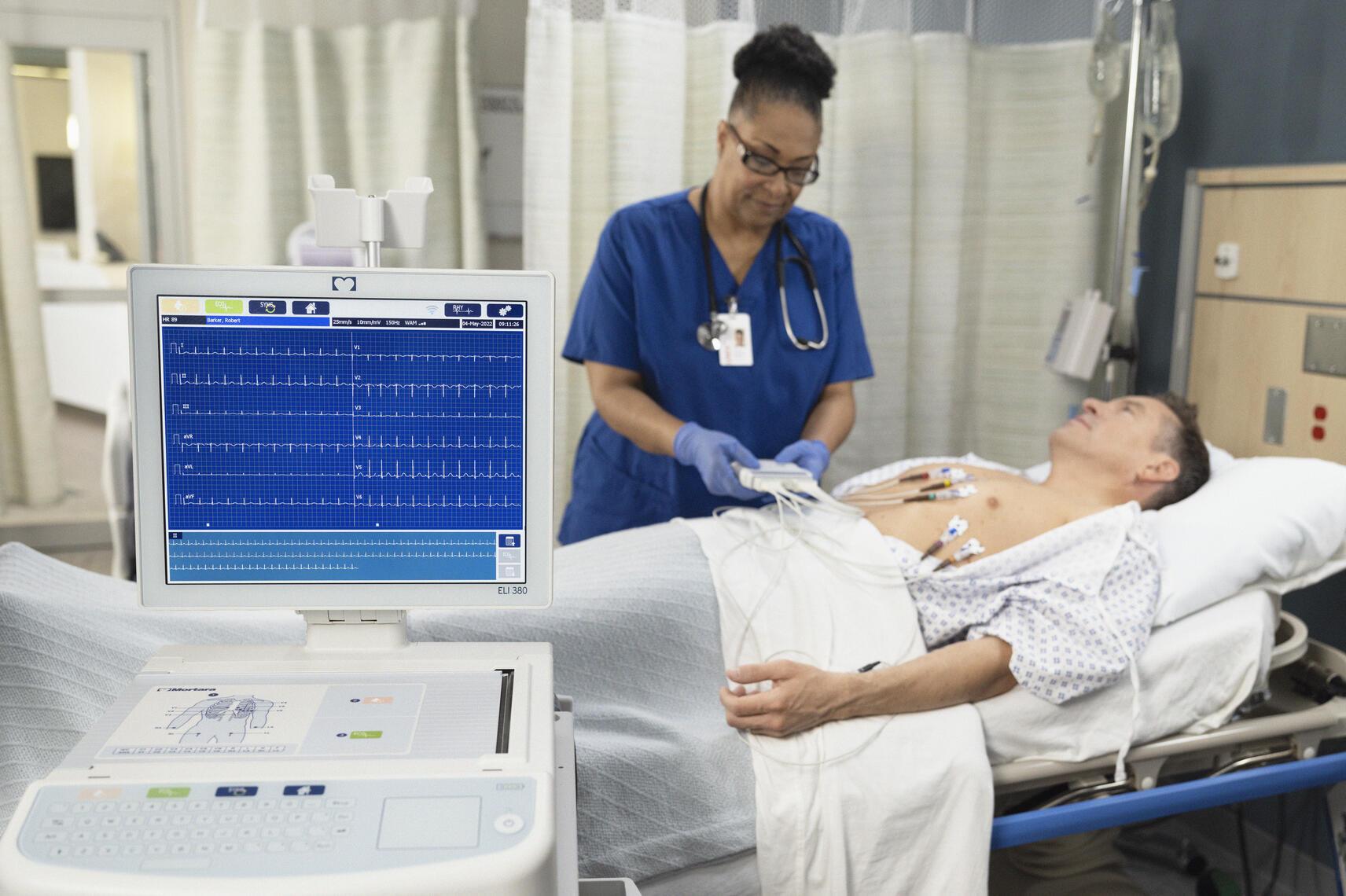
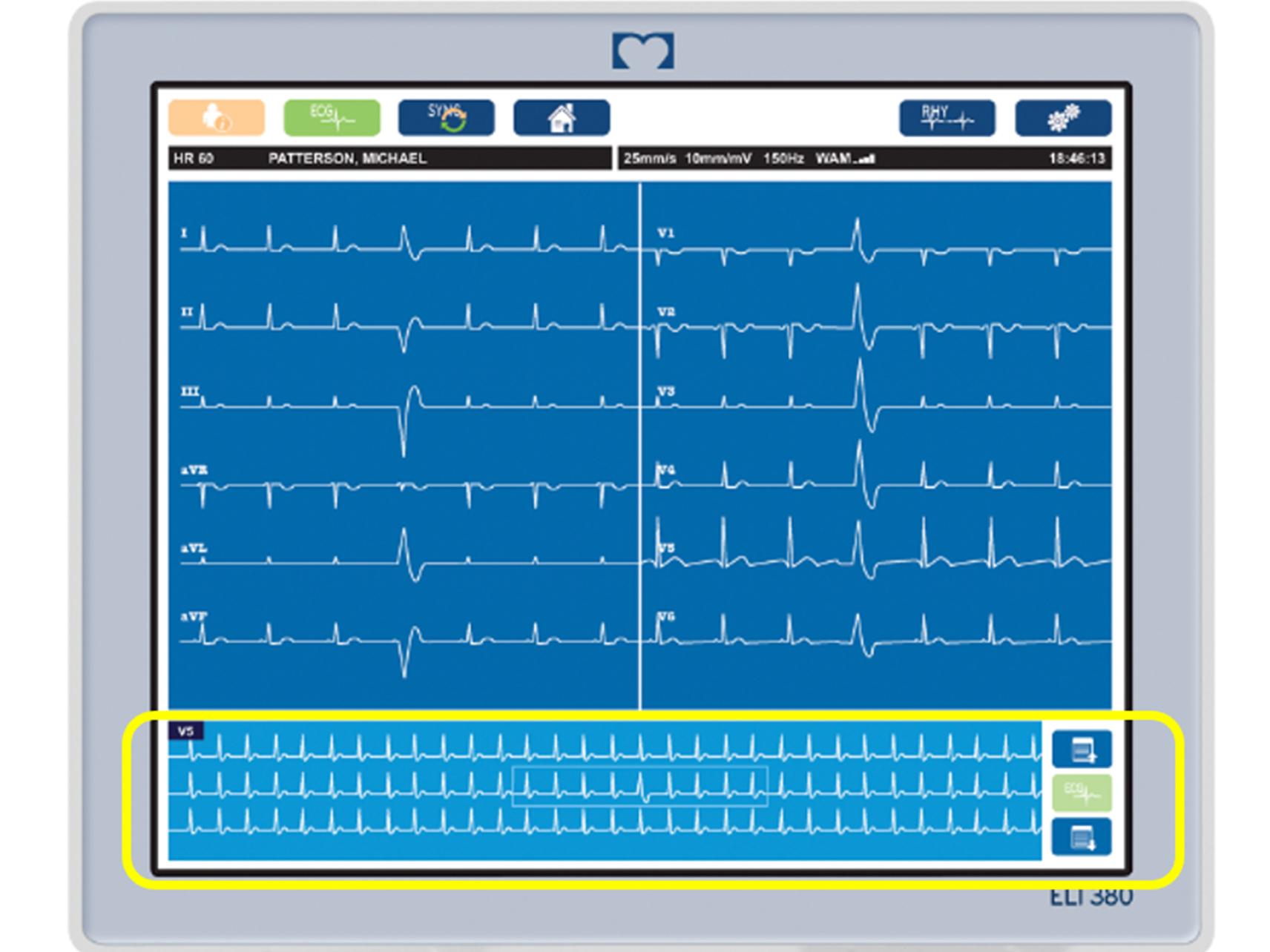
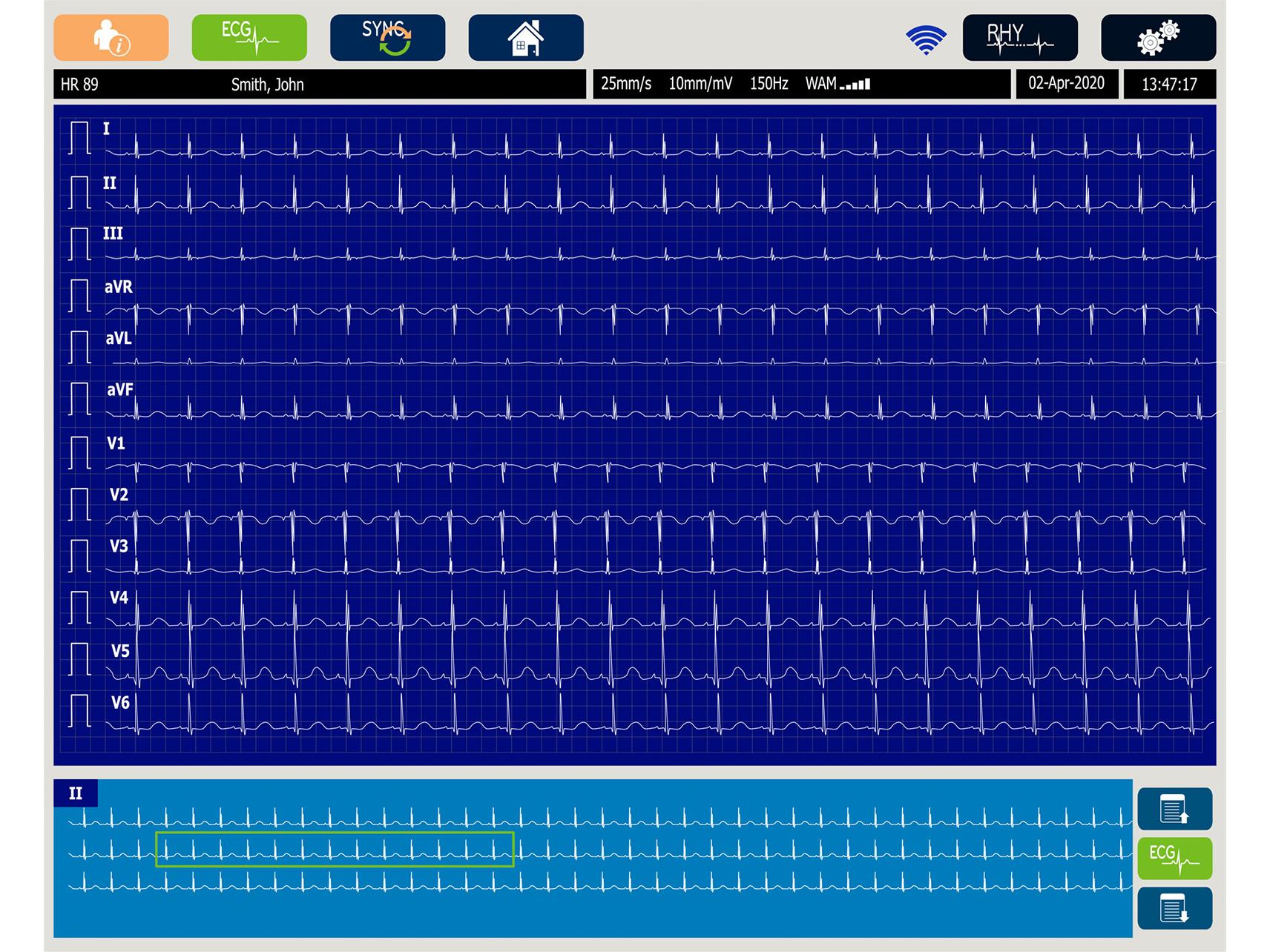
- Preventing Repeat ECGs