Overview
Features
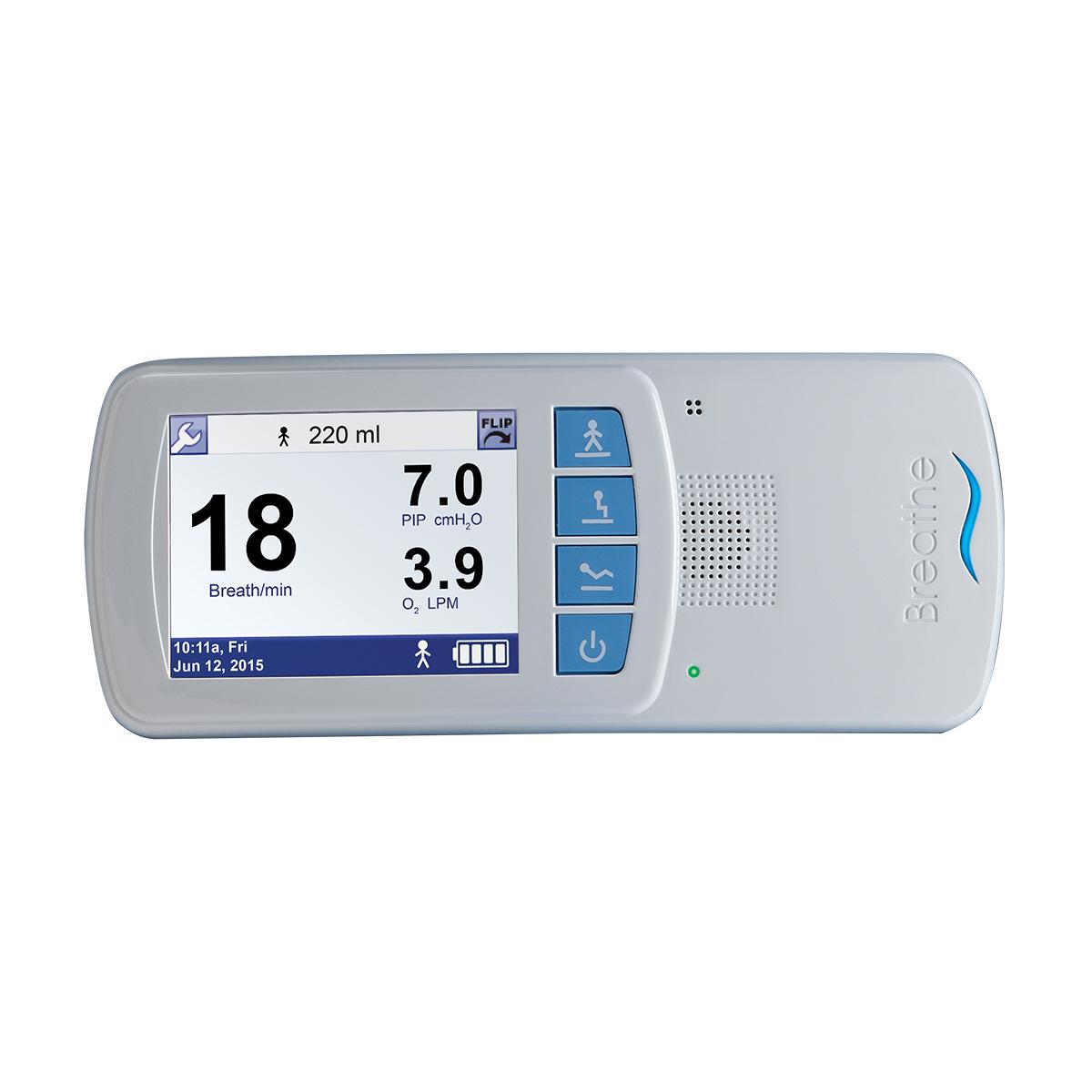
Wearable
This home ventilator device features a belt clip and a carry case.
Modular
The Life2000 System can be conveniently used at home or on the go.
Mask-Free
The Breathe Pillows Interface provides non-invasive ventilation.
Breathe Pillows Interface

The Life2000 Ventilation System is available with comfortable and discreet Breathe Pillows Interface.
Small-diameter tubing (5mm vs. traditional 22mm)
Patients can talk while wearing the noninvasive Breathe Pillows Interface
Available in multiple sizes
Breathe UNIVERSAL CIRCUIT Connector

The Life2000 Ventilation System features a circuit that is compatible with virtually any third-party interface (including full face mask, tracheostomy tube, and intubation tube).
Ability to switch masks throughout the day and night
Allows for an easy transition to home from hospital/acute settings
Versatile configurations and adjustable settings for continuous ventilation

The Life2000 Ventilation System provides three configurations for optimal versatility:
Stationary
Wearable inside the home with extended range - small-diameter, up-to-50-foot tubing allows for easy mobility
Wearable outside the home as stand-alone ventilation with an alternate pressure source
Patient-selectable prescription settings

Three patient-selectable prescription settings for rest, moderate, or high activity
Allows for continuous, around-the-clock use
Adaptable to patients’ ventilatory demands and breathing patterns
Reimbursement and support
The Life2000 Ventilation System is covered by Medicare and commercial insurance plans for invasive and non-invasive ventilators.
HCPCS Codes: E0465 and E0466
Our team of respiratory therapists work directly with physicians and other healthcare providers to ensure the Life2000 Ventilation System supports optimal clinical outcomes.
How has the LIFE2000 Ventilation System changed lives?
Rx Only. For safe and proper use of product mentioned herein, please refer to the Instructions for Use or Operator Manual.
US-FLC100-240013 (v1.0) 12/2024
Technical Specifications
Dig deeper into product attributes to see how we can fit your requirements.
| Ventilation Modes | Assist, Assist/Control, Control with Apean backup |
| Breathing Type | Mandatory or Assisted |
| Tidal Volume | Up to 2000 mL (via Venturi effect) |
| Maximum Positive Inspiratory Pressure (PIP) | 40 cmH2O |
Education & Documentation
Get in the know to get the most value out of your solution.
Learn how the LIFE2000 Ventilation System supports breathing.
View this intro to the LIFE2000 Ventilation System's capabilities and configurations.
How to use: Introduction
How to use: Extended Range Configuration
How to use: Stand-Alone Configuration
How to use: Cleaning & Maintenance
How to use: Titration
How to use: Alarms & Troubleshooting
Product Documentation
-
Coverage Criteria
keyboard_arrow_downLIFE2000 Coverage Criteria Flyer
-
Can the LIFE2000 Ventilation System be used away from home?
keyboard_arrow_downYes. The device may be connected to an oxygen cylinder with a 50 PSI, ≥ 40 LPM at 41 PSI regulator for respiratory support outside the home.
-
How long is the LIFE2000 Ventilation System's battery life?
keyboard_arrow_downIn normal use, the battery's charge lasts approximately 5 to 6 hours.
-
What interface is available with the LIFE2000 Ventilation System?
keyboard_arrow_downThe unit uses our mask-free Breathe Pillows Interface. It's available in four sizes—XS, S, M, and L—and is fitted to the patient during set-up.
-
What is PROPORTIONAL OPEN VENTILATION (POV) technology?
keyboard_arrow_downPOV technology refers to the method used to ventilate the patient. The interface's Venturi system entrains room air which, combined with the device's set volume and your patient's own effort, yields its total delivered tidal volume.
-
Can the LIFE2000 Ventilation System be used during the day and at night?
keyboard_arrow_downThe device can be used day or night, or both, and the prescribing clinician may indicate how they wish the patient to use the device.
Frequently Asked Questions
Expand AllRx Only. For safe and proper use of product mentioned herein, please refer to the Instructions for Use or Operator Manual.
US-FLC100-240013 (v1.0) 12/2024